Anti-NMDA receptor encephalitis may affect both children and adults, and have them develop various symptoms including psychosis etc. The encephalitis is one of autoimmune neurological diseases. The immune system of a patient produces pathogenic autoantibodies that bind to NMDA receptors in their brain and cause the disease. Early intervention is expected to prevent residual complications and to promote early recovery to their own lives. For the definite diagnosis of Anti-NMDA receptor encephalitis, autoantibody detection is necessary. However, the antibody analysis is not available in some areas or countries, and at times physicians need to wait for a while to obtain the results, which may delay administration of appropriate immunomodulatory treatment. Based on this issue, clinical diagnostic criteria were proposed in 2016, which allow us to diagnose probable anti-NMDA receptor encephalitis regardless of the antibody status. The criteria consist of 6 major symptom groups derived from the past reports, and majority of these evidences are from adults with the encephalitis. We therefore evaluated the validity of the criteria for anti-NMDAR encephalitis in a Japanese pediatric cohort by collaborating with Japanese child neurologists.
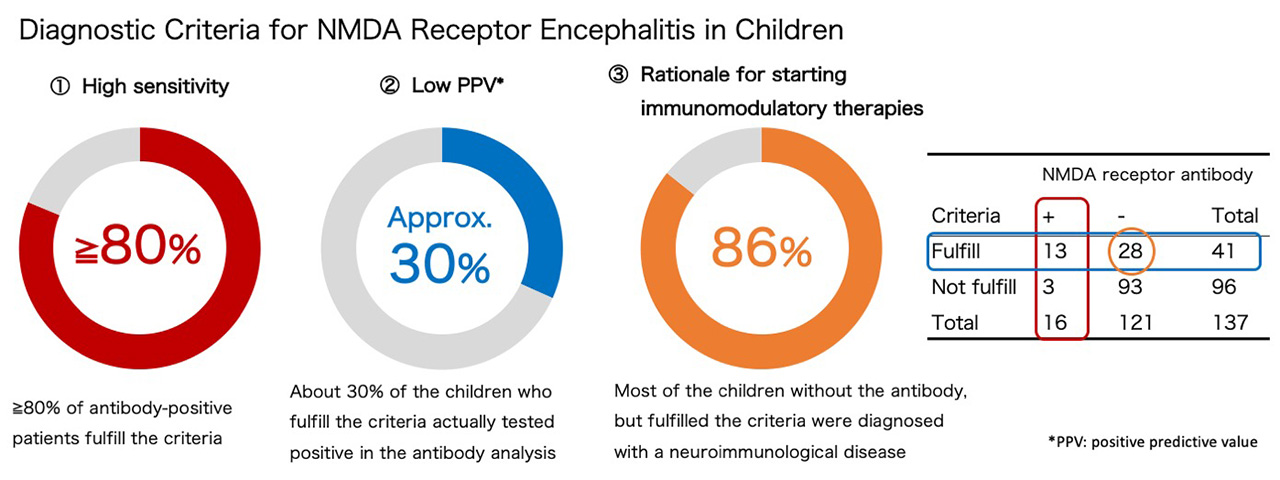
Three major findings in our report regarding the criteria are as follows:
Collectively, we concluded that the 2016 diagnostic criteria are useful and reliable for deciding to start immunomodulatory therapy in the criteria-positive cases. However, the antibody test is necessary to confirm diagnosis of anti-NMDA receptor encephalitis.
This report will help physician decide starting early and aggressive immunomodulatory therapy on the criteria positive children, and might improve their outcomes, accordingly. We truly appreciate all the child neurologists who have kindly cooperated to this study by providing clinical information, while their working hard as child health care providers. We hope our study will be of benefit to save children and their lives.